Our skin is not just a protective shield; it's a mirror reflecting our overall health. Skin conditions such as psoriasis, eczema, and acne are not merely surface irritations but often the external manifestations of internal imbalances. So, what’s the common denominator? Inflammation.
A number of seemingly disparate skin issues share a common thread – but why? And what is inflammation? This natural immune response is triggered by the body to protect itself from harmful invaders. That’s not so bad, right? It’s all well and good until this response goes awry, leading to chronic inflammation, and all the diseases that accompany this state, from obesity and heart disease to inflammatory skin conditions.
Psoriasis

Psoriasis is characterised by red, scaly patches on the skin, resulting from the rapid overproduction of skin cells. Inflammation plays a key role in psoriasis, as it activates an immune response that speeds up skin cell turnover. Immune cells mistakenly attack healthy skin cells, leading to the characteristic plaques and discomfort.
Psoriasis can occur on any part of the body, but it commonly affects areas like the elbows, knees, scalp, and lower back. The severity of psoriasis varies from mild, with only a few small patches, to severe, with large areas of skin affected. It’s a chronic condition, meaning it can persist for a long time or even throughout a person's life, and while there is no cure, various treatments can help manage the symptoms and control flare-ups. These treatments may include topical creams, phototherapy (light therapy), oral medications, and biologic drugs that target specific components of the immune system. Take a look at the 7 types of psoriasis:
- Plaque Psoriasis: Plaque psoriasis is the most common form, accounting for about 80-90% of all psoriasis cases. It appears as raised, red patches covered with thick, silvery-white scales. These patches can be itchy, painful, and may crack or bleed.
- Guttate Psoriasis: Guttate psoriasis often develops in childhood or early adulthood and is characterised by small, drop-like lesions on the skin. These lesions are typically red or pink and may be widespread across the body.
- Inverse Psoriasis: Inverse psoriasis affects areas where skin touches skin, such as the armpits, groin, and under the breasts. It appears as smooth, red, inflamed patches and is more common in individuals who are overweight.
- Pustular Psoriasis: Pustular psoriasis is characterised by small, pus-filled blisters surrounded by red skin. The blisters can be painful and may occur on localised areas or across the body.
- Erythrodermic Psoriasis: This is a severe and rare form of psoriasis that can cover the entire body with a red, peeling rash. Erythrodermic psoriasis can be life-threatening and requires immediate medical attention.
- Scalp Psoriasis: Scalp psoriasis affects the scalp and may extend to the forehead, back of the neck, and behind the ears. It can cause red, scaly patches and may lead to flaking and itching.
- Nail Psoriasis: Nail psoriasis affects the fingernails and toenails, causing changes in the appearance of the nails, such as pitting, discolouration, thickening, and separation from the nail bed.
Eczema

Eczema, or atopic dermatitis, is marked by itchy, inflamed skin. It is primarily an allergic condition driven by an immune system overreaction to irritants or allergens. This hyperactive immune response leads to inflammation in the skin, causing redness, itching, and the eventual breakdown of the skin's protective barrier. Also known as atopic dermatitis, this chronic skin condition can range from mild to severe and is characterised by periods of flare-ups and remission. Eczema is believed to be caused by a combination of genetic and environmental factors, making it more common in individuals with a family history of allergic conditions like asthma or hay fever. The exact cause of eczema is not fully understood, but it is related to an overactive immune response and a compromised skin barrier, which allows irritants, allergens, and bacteria to penetrate the skin more easily.
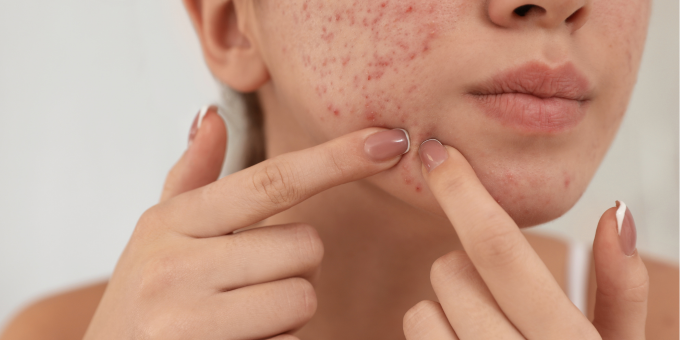
Acne
Up to 85% of Aussies will experience acne at some stage in their life, with 5% reporting severe cases. But it’s not just teenagers! Around 50% of people go on to experience acne in their 30s – if this is hitting home for you, know that you’re not alone. At different stages of life, people go through some big hormonal changes, from puberty to menopause or andropause, all of which can cause pH imbalances in the skin, poor blood circulation and excessive oil production, Acne, particularly in its more severe forms, is characterised by inflamed pimples, pustules, and cysts, and inflammatory responses within hair follicles are at the heart of acne development. Bacteria, oil production, and dead skin cells can trigger this inflammation, leading to painful and unsightly breakouts.
Common Triggers

Diet: Certain foods, especially those high in sugar, processed ingredients, and unhealthy fats, can trigger inflammation. A balanced, anti-inflammatory diet can benefit all three conditions. Research has suggested that sugar may contribute to the development of acne in several ways – one such way is by increasing insulin levels in the body. Insulin is a hormone that regulates blood sugar levels, but it can also stimulate the production of androgens, which are hormones that can increase oil production in the skin. Excess oil production can lead to clogged pores and the development of acne. Excess sugar consumption may also increase to inflammation in the body, which can exacerbate acne as it causes skin to produce more oil, leading to clogged pores. We also know that too much sugar can affect the balance of bacteria in the gut, which can have a significant impact on the health of the skin – not to mention the whole body! Excessive sugar consumption can lead to an overgrowth of harmful bacteria, such as certain strains of Clostridium and Enterococcus. These harmful bacteria thrive on sugar and can outcompete beneficial bacteria in the gut. A healthy gut microbiome is essential for overall health, so when things get thrown off, it can lead to a spike in acne breakouts.
Let’s take a look at a few more ways sugar leaves you susceptible to skin conditions:
- Glycation: When sugar enters your bloodstream, it can attach to proteins, including collagen and elastin, which are essential for maintaining skin's elasticity and firmness. This process is called glycation. When sugar molecules bind to these proteins, they form advanced glycation end products (AGEs), which can lead to skin ageing, wrinkles, and a loss of skin elasticity.
- Hormonal Imbalance: Sugar consumption can affect hormone levels, particularly insulin and insulin-like growth factor (IGF-1). Higher levels of IGF-1 are associated with increased oil production in the skin's sebaceous glands. Excess oil can clog pores, leading to acne breakouts.
- Weakening of the Skin Barrier: A diet high in added sugars can weaken the skin's natural barrier. The skin barrier is responsible for keeping irritants out and retaining moisture. When this barrier is compromised, it becomes easier for allergens, pollutants, and irritants to penetrate the skin, leading to inflammatory reactions and skin conditions such as eczema.
Stress: Chronic stress can wreak havoc on the immune system and exacerbate inflammation. Stress management techniques like meditation and exercise can help.
Microbiome: The gut and skin microbiome play a crucial role in inflammation. Maintaining a healthy gut and using gentle, skin-friendly products can help restore balance.
Allergens: Identifying and avoiding allergens specific to your condition is vital. Eczema sufferers may react to certain fabrics, while acne-prone individuals may be sensitive to pore-clogging ingredients.
Managing Inflammation for Healthy Skin
Topical Solutions: Depending on the condition, using appropriate topical treatments can help manage symptoms while you aim to get your gut microbiome back in order. For psoriasis, moisturisers and anti-inflammatory creams may be beneficial. Eczema patients can benefit from emollients, while acne sufferers may find success with spot treatments and gentle cleansers.
Lifestyle Adjustments: Adopt a balanced, anti-inflammatory diet rich in fruits, vegetables, and omega-3 fatty acids. Manage stress through meditation, yoga, or deep-breathing exercises.

Supplements: Some supplements, like omega-3 fatty acids and probiotics, can help reduce inflammation and improve skin conditions. Consult a healthcare professional before incorporating supplements into your routine.
Psoriasis, eczema, and acne may manifest on the skin's surface, but their roots lie in inflammation. Understanding the commonality of inflammation in these conditions allows us to adopt holistic approaches to manage and alleviate symptoms. By addressing the root causes, adopting a balanced lifestyle, and seeking professional guidance, we can support healthier, happier skin and overall wellbeing.
Need a little help getting your health back on track? Join us for the 8-Week Program and we’ll help you change the way you look at food – and that doesn’t mean you have to follow restrictive diets or miss out on your favourite foods; we believe you can still enjoy delicious food without jeopardising your health. With celebrity chef Sarah Glover on our panel of experts, you’ll have an array of fun recipes at your fingertips, along with our own exclusive armoury of simple, tasty and healthy recipes for everything from daily meals to impressive entertaining. We know it can be hard to stick to your health goals – especially when you’re trying to manage it alone. When you sign up with us, you’ll have access to clear-cut meal plans, community support and exclusive access to our sugar-free content. Here’s what’s on offer:
- 8 weeks of meal plans and shopping lists.
- 90+ member-only recipes.
- Community forums to share your journey.
- Support and guidance from the I Quit Sugar team.
- Exclusive content from our panel of experts.
So, if you’re ready to ditch sugar and the host of maladies that come with it, it’s not too late to join. We’d love to help you get started on your health journey. Sign up HERE today!