There’s nothing sunny about an outbreak of scaly, itchy, burning psoriasis – but researchers have found an interesting link between low levels of the sunshine vitamin and the severity of symptoms. With Psoriasis Action Month upon us, it’s time we unpack what the condition entails, along with the risk factors and the latest news on what really causes this notorious rash.
First for the 411 on what’s new – recent research has found that a vitamin D deficiency is extremely common among those with psoriasis, with researchers specifically highlighting that levels of over 30 ng/ml could significantly reduce the severity of symptoms of the condition, along with a host of other autoimmune diseases. The study found that a whopping 60% of psoriasis patients were deficient in the sunshine vitamin, compared to just 17.5% of those without the condition. Now this isn’t to say low vitamin D levels cause psoriasis – unfortunately, we’ve yet to pin down an exact cause – but there is a strong link between the two.

But what exactly is the link, you ask? Well, another study suggests that it’s actually the chronic inflammation associated with psoriasis that promotes low vitamin D levels, along with a general loss of nutrient absorption that comes with the territory. But the encouraging conclusion of that first study is that early detection of deficiency in vitamin D could result in better outcomes for psoriasis patients – this means treating the deficiency before it gets out of hand.
Before we dive further into the theories around the causes of psoriasis, let’s jump into what psoriasis actually is.
What Exactly is Psoriasis?
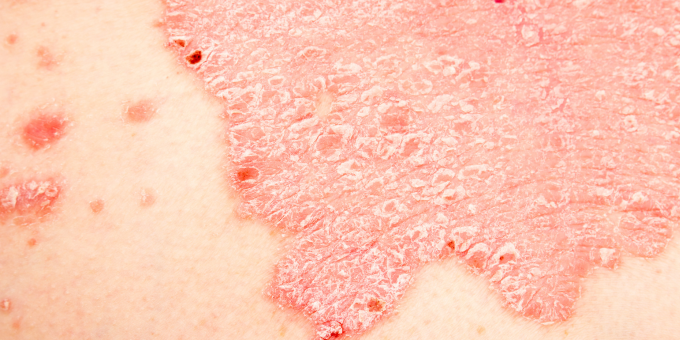
Psoriasis is a chronic autoimmune skin condition that causes the rapid buildup of skin cells. Normally, skin cells grow deep within the skin and rise to the surface over the course of a few weeks. In psoriasis, this process is significantly accelerated, leading to the accumulation of skin cells on the surface. These excess skin cells form thick, silvery scales and red patches that are often itchy, painful, and may crack or bleed. Psoriasis can occur on any part of the body, but it commonly affects areas like the elbows, knees, scalp, and lower back. The severity of psoriasis varies from mild, with only a few small patches, to severe, with large areas of skin affected. It’s a chronic condition, meaning it can persist for a long time or even throughout a person's life, and while there is no cure, various treatments can help manage the symptoms and control flare-ups. These treatments may include topical creams, phototherapy (light therapy), oral medications, and biologic drugs that target specific components of the immune system. Take a look at the 7 types of psoriasis:
- Plaque Psoriasis: Plaque psoriasis is the most common form, accounting for about 80-90% of all psoriasis cases. It appears as raised, red patches covered with thick, silvery-white scales. These patches can be itchy, painful, and may crack or bleed.
- Guttate Psoriasis: Guttate psoriasis often develops in childhood or early adulthood and is characterised by small, drop-like lesions on the skin. These lesions are typically red or pink and may be widespread across the body.
- Inverse Psoriasis: Inverse psoriasis affects areas where skin touches skin, such as the armpits, groin, and under the breasts. It appears as smooth, red, inflamed patches and is more common in individuals who are overweight.
- Pustular Psoriasis: Pustular psoriasis is characterised by small, pus-filled blisters surrounded by red skin. The blisters can be painful and may occur on localised areas or across the body.
- Erythrodermic Psoriasis: This is a severe and rare form of psoriasis that can cover the entire body with a red, peeling rash. Erythrodermic psoriasis can be life-threatening and requires immediate medical attention.
- Scalp Psoriasis: Scalp psoriasis affects the scalp and may extend to the forehead, back of the neck, and behind the ears. It can cause red, scaly patches and may lead to flaking and itching.
- Nail Psoriasis: Nail psoriasis affects the fingernails and toenails, causing changes in the appearance of the nails, such as pitting, discolouration, thickening, and separation from the nail bed.
The Cause of Psoriasis

The exact cause of psoriasis is not fully understood, but researchers believe that it is a complex interplay of genetic, immune system, and environmental factors. Several theories have been proposed as potential contributors:
Genetic Predisposition: Psoriasis has a strong genetic component, and a family history of the condition increases the risk of developing it. Specific genetic variations have been linked to an increased susceptibility to psoriasis.
Immune System Dysfunction: Psoriasis is considered an autoimmune disease, where the immune system mistakenly attacks healthy skin cells, leading to inflammation and rapid cell turnover. T cells, a type of immune cell, are believed to play a significant role in the inflammatory process.
Environmental Triggers: Certain environmental factors can trigger or exacerbate psoriasis in individuals with a genetic predisposition. Triggers may include stress, infections, injuries to the skin, smoking and certain medications.
Immune Response to Skin Microbes: Some researchers propose that psoriasis may be triggered by an abnormal immune response to skin microbes, such as bacteria or fungi.
Epigenetics: Epigenetic changes, which are alterations in gene expression without changes in the DNA sequence, may also contribute to the development of psoriasis in susceptible people.
Stress: Stress and mental health factors, such as anxiety and depression, can worsen psoriasis symptoms. They may not be the root cause, but they can trigger or exacerbate flare-ups.
Lifestyle Factors: Unhealthy lifestyle habits, such as smoking, excessive alcohol consumption, and poor diet, may also play a role in the development and severity of psoriasis. Excess sugar consumption has also been linked to the condition as refined sugars and high-glycaemic foods can lead to chronic inflammation in the body. Psoriasis is an inflammatory skin condition, after all, so anything that promotes inflammation may worsen psoriasis symptoms – and trust us, added sugar is the king of inflammation!

High sugar intake can contribute to insulin resistance, a condition in which cells become less responsive to insulin, which may also be linked to the development or severity of psoriasis. Too much of the sweet stuff can negatively affect gut health by promoting the growth of harmful bacteria and yeast – and yep, you guessed it, an unhealthy gut microbiome is linked to inflammatory skin conditions like psoriasis.
It's important to note that psoriasis is a multifactorial condition, meaning that multiple factors likely interact to contribute to its development and progression. Research in this field is ongoing, and there is still much to learn about the precise mechanisms underlying psoriasis. But, as you can see, new research is coming in and it just may change the way we approach and treat psoriasis.
Keen to improve your gut health and reduce inflammation? The IQS team have something special for you. Our ALL NEW 21-Day Gut Rebalance Program kicks off soon with delicious, nourishing recipes and exclusive expert content to support you on your way to better health. Whether it's constipation, bloating or even stress that's got you down, it could be your gut warning you that you're missing out on the gut-nourishing foods that help us thrive. We'll show you the ins and outs of healing, from the benefits of probiotics and prebiotics to the inflammation-busting foods you should be eating. Take a look at some of the exciting new recipes on the program:
- Pork Kimchi Dumplings
- Homemade Sourdough Bread
- Miso-Baked Salmon
- Tempeh Satay
- Chinese Beef + Broccoli
- Chocolate Chia Smoothie Bowl
And that's not even scratching the surface! We're selling out fast so don't wait, sign up now!