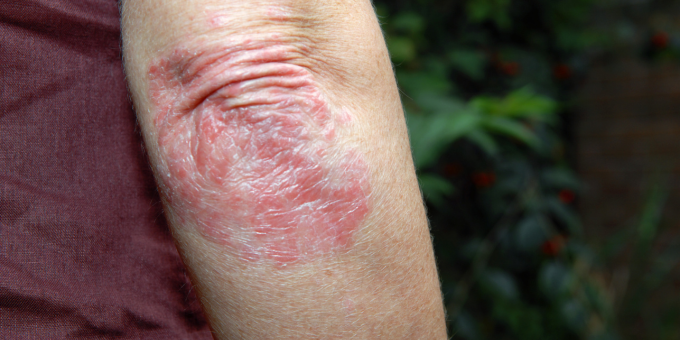
There is more than meets the eye with this frustrating autoimmune condition – underneath the skin, uncontrolled inflammation in the body is raising your risk for a number of other conditions, from heart disease to arthritis. Here’s what you need to know, and why holistic treatment is vital for psoriasis.
Our IQS 8-Week Program is designed to help you reduce your sugar intake and been proven to significantly reduce fatigue, inflammation, gut issues, bad skin, bad sleep and SO MUCH MORE! It's because we give you the full tool kit to help you learn more about sugar, what it does to your body and why you should care. Plus, it's delicious! You get full weekly meal plans, recipes, motivation, expert advice and more to help you on your journey to better health. Sign up HERE!
Psoriasis, a chronic skin condition characterised by red, scaly patches, is more than what meets the eye. While the visible lesions may be the tip of the iceberg, lurking beneath the surface is a complex interplay of factors that extend beyond the skin. Inflammation may be weaving a web of potential risks, known as comorbidities. Let's delve into the hidden depths of psoriasis and understand why this skin disease might be signalling something more concerning.
The Skin's Story

Psoriasis manifests on the skin, causing discomfort and sometimes pain for those affected. The visible symptoms, however, are just one chapter in the skin's story. Beneath the surface, a deeper narrative unfolds, driven by inflammation – the body's response to an immune system gone awry. But, before we unpack the implications of inflammation, what exactly is psoriasis? It’s a chronic autoimmune skin condition that causes the rapid buildup of skin cells. Normally, skin cells grow deep within the skin and rise to the surface over the course of a few weeks. In psoriasis, this process is significantly accelerated, leading to the accumulation of skin cells on the surface. These excess skin cells form thick, silvery scales and red patches that are often itchy, painful, and may crack or bleed. Psoriasis can occur on any part of the body, but it commonly affects areas like the elbows, knees, scalp, and lower back. The severity of psoriasis varies from mild, with only a few small patches, to severe, with large areas of skin affected. Plaque psoriasis is the most common form, accounting for about 80-90% of all psoriasis cases, and it appears as raised, red patches covered with thick, silvery-white scales. These patches can be itchy, painful, and may crack or bleed, but there are a number of other forms of the disease.

It’s a chronic condition, meaning it can persist for a long time or even throughout a person's life, and while there is no cure, various treatments can help manage the symptoms and control flare-ups. These treatments may include topical creams, phototherapy (light therapy), oral medications, and biologic drugs that target specific components of the immune system.
Beyond its impact on the skin, inflammation associated with psoriasis can extend its reach throughout the body. This chronic inflammation is more than an inconvenience; it's a potential precursor to various comorbidities that can affect different organs and systems.
The Hidden Risks and Comorbidities
Cardiovascular Complications: Psoriasis has been linked to an increased risk of cardiovascular diseases, including heart attacks and strokes. The inflammatory state in psoriasis may contribute to the development of atherosclerosis, narrowing blood vessels and affecting heart health.
Metabolic Syndrome: Psoriasis has been associated with metabolic syndrome, a cluster of conditions that includes obesity, high blood pressure, elevated cholesterol levels, and insulin resistance. These factors collectively increase the risk of diabetes and heart disease.
Joint Involvement - Psoriatic Arthritis: A significant number of individuals with psoriasis may develop psoriatic arthritis, a condition affecting the joints. The inflammation that starts in the skin can extend to the joints, causing pain, stiffness, and potentially leading to joint damage.
Mental Health Impact: The visible nature of psoriasis lesions can have a profound impact on mental health. Depression and anxiety are common comorbidities, highlighting the importance of addressing the emotional toll of the condition.
In the realm of psoriasis and psoriatic arthritis (PsA), ongoing research has paved the way for innovative treatments, thanks to the swift progress of modern technology. Over the past decade, numerous treatments have entered the market, with more on the horizon. The spectrum of effective therapies spans from topical and phototherapy to biologics and oral systemics, complemented by supportive roles of complementary medicine. The complexity arises as some treatments can be combined, potentially overwhelming individuals navigating their options. Beyond addressing the visible lesions, the focus is on holistic care, recognising that psoriasis involves more than skin-deep challenges.
Michael Lewitt, dermatologist from the Illinois Dermatology Institute and a member of the National Psoriasis Foundation (NPF) Medical Board, tells the National Psoriasis Organisation why there is usually more to psoriasis than meets the eye, highlighting that the visible lesions on the skin are not the full story.
“Under the skin, inflammation throughout the body is putting you at risk of developing related conditions, called comorbidities,” he says. “Treating psoriasis above and below the skin is essential, because the comorbidities of psoriasis include high blood pressure, type 2 diabetes, and PsA, among others.”

Psoriasis may be a skin disorder, but its implications are far-reaching. The inflammatory undercurrent can set the stage for a variety of comorbidities, emphasising the need for a holistic approach to management. Understanding the hidden risks allows individuals with psoriasis to take proactive steps, not only for their skin but for their overall well-being. Seeking comprehensive care that addresses both the visible symptoms and the concealed risks can empower individuals to navigate the complex landscape of psoriasis with resilience and vitality.
Holistic treatment for psoriasis involves addressing the condition from multiple angles, considering both the visible symptoms on the skin and the underlying factors contributing to inflammation. Here are some approaches to holistic psoriasis care.
Topical Treatments: Use topical creams or ointments prescribed by your dermatologist to directly target skin lesions.
Phototherapy (Light Therapy): Phototherapy involves exposing the skin to ultraviolet (UV) light under medical supervision. This can help reduce inflammation and slow down the rapid skin cell growth associated with psoriasis.
Systemic Medications: Biologics and oral medications may be prescribed to modulate the immune system and manage inflammation. These are typically recommended for moderate to severe cases.
Complementary and Alternative Medicine (CAM): Explore complementary therapies such as acupuncture, yoga, or meditation to manage stress, which can trigger or exacerbate psoriasis.
Dietary Changes: Adopt an anti-inflammatory diet rich in fruits, vegetables, whole grains, and lean proteins. Omega-3 fatty acids from sources like fish or flaxseed may also be beneficial. It’s also vital to avoid inflammatory foods like trans fats, excess added sugar and fast food.
Maintain a Healthy Lifestyle: Regular exercise and maintaining a healthy weight can positively impact psoriasis. Smoking and excessive alcohol consumption may worsen symptoms, so quitting these habits is advisable.
Stress Management: Practice stress-reducing techniques like mindfulness, deep breathing, or engaging in hobbies to minimise stress, a common trigger for psoriasis flare-ups.
Regular Check-ups: Schedule regular follow-ups with your dermatologist to monitor your condition and adjust treatment plans as needed.
Always consult with your healthcare provider before making significant changes to your treatment plan or lifestyle. Personalised care is essential, and your healthcare team can guide you toward the most effective and sustainable holistic approach for your specific situation.
Need a little help getting your health back on track? Join us for the 8-Week Program and we’ll help you change the way you look at food – and that doesn’t mean you have to follow restrictive diets or miss out on your favourite foods; we believe you can still enjoy delicious food without jeopardising your health. With celebrity chef Sarah Glover on our panel of experts, you’ll have an array of fun recipes at your fingertips, along with our own exclusive armoury of simple, tasty and healthy recipes for everything from daily meals to impressive entertaining. We know it can be hard to stick to your health goals – especially when you’re trying to manage it alone. When you sign up with us, you’ll have access to clear-cut meal plans, community support and exclusive access to our sugar-free content. Here’s what’s on offer:
- 8 weeks of meal plans and shopping lists.
- 90+ member-only recipes.
- Community forums to share your journey.
- Support and guidance from the I Quit Sugar team.
- Exclusive content from our panel of experts.
So, if you’re ready to ditch sugar and the host of maladies that come with it, it’s not too late to join. We’d love to help you get started on your health journey. Sign up HERE today!